Haemodialysis
Part One
There are two main dialysis options
Haemodialysis
This dialysis option is the focus of this website and will be discussed hereafter in detail
But first …
Please Note … although this website does not discuss peritoneal dialysis in any detail, it is an excellent dialysis choice for many patients.
In our own program, 20-25% of our patients use peritoneal dialysis. Of these, a little over half now use overnight, automated peritoneal dialysis.
Peritoneal dialysis, though NOT the focus of this website, is both a home therapy and, at least potentially for most, an overnight one too.
You should discuss the peritoneal dialysis options with your dialysis unit.
Further useful information on it can be found at:
http://www.kidney.org/kls/patients/plu_pd/pd_3.cfm
Or, to learn about overnight home peritoneal dialysis (APD), try…
http://kidney.niddk.nih.gov/kudiseases/pubs/peritoneal/
From now on, however, the focus of this website is entirely on haemodialysis.
This is
not intended to represent bias – it simply means that this site is intent
on one task alone – to explain the processes of haemodialysis and to
introduce you to nocturnal home haemodialysis.
Haemodialysis
There are several haemodialysis options. It is important to note that the terminology that is used will vary a little - country to country
Choices also depend upon both availability and geography
… That having been said, the three main choices are:
Limited care ‘satellite’ haemodialysis
For most patients on dialysis, haemodialysis has, by ‘convention’, always been: 4 hours, 3 times/week (or some near variant). From here on at this website, this will be called ‘4x3 HD’
Worldwide, dialysis time per session varies significantly
The average sessional duration in the US is still less than 4 hours and closer to 3 ½ hours.
In other countries and regions, sessional duration is more commonly in excess of 4 hours and in Australia, closer to 4 ½ hours while Japan is closer to 5 hours.
Individual facility-based treatment duration is rarely greater than 5 hours
Worldwide, dialysis is routinely prescribed only three times per week and thus forces a ‘long break’ on all facility-based patients doing conventional 3x4 HD
BUT … have you ever asked yourself – WHY?
There are three important questions
1. Is haemodialysis practice based on good science?
2. Are there smarter, newer technologies around?
3. Might newer approaches produce better outcomes for patients?
And … there is a fourth and important question – at least, it is a key question for governments and funding agencies …
4. Can better dialysis be delivered yet at lower cost to the provider (i.e. governments and taxpayers)?
When kidneys fail
They almost always fail permanently and fail in all their functions …
Little or diminishing waste excretion occurs
Little or diminishing fluid excretion occurs
Little or diminishing ‘other functions’ occur
This means that all (or most) wastes ‘stay on board’ and all (or most) fluid swallowed stays inside the body which inevitably …
Swells the blood volume
Raises the blood pressure
Stretches the heart and blood vessels
Question …
So … how do we replace the functions of this usually continuingly functioning ‘vital’ organ?
Answer …
At the moment, we use artificial kidney treatment (standard, conventional dialysis) for an average total of 12 hours out of the 168 hr week
… or 7% of the time
This is to replace the function of an organ system used to running, in the background, 24 hours a day, 7 days a week
… or 100% of the time
Question …
Is this enough?
Answer …
Standard dialysis practice - (4x3 HD)
Is currently performed, in most places round the world, for 4-5 hrs dialysis on Mon/Wed/Fri or Tues/Thurs/Sat … with Sundays off!
This means that …
In 4-5 hrs, all wastes and fluids gained must be removed
This results in a 2nd/3rd daily ‘assault’ on body biochemistry and blood volume
No wonder so many on 4x3 HD feel like they have been run over by a steamroller every other day
So … what governs good dialysis?
Dialyser surface area (m2)
Blood flow rate (pump speed)
Dialysate flow rate
… these factors are easy and popular to adjust … but are relatively ineffective
Dialysis Time
Dialysis Frequency
… these factors are also easy but unpopular to adjust … but are very effective
In my view … ‘optimal’ dialysis should be …
24 hrs/day, 7 days/wk – just as a pair of normal kidneys would provide - but no-one wants to depend on a machine like that!
Humans must live, react, inter-act, work, play, love, laugh, weep, enjoy, thrill … all in their waking hours
Yet, currently, we hook our patients up to dialysis machines in their waking hours, just when they should be doing their ‘living’ things
So, it stands to reason that optimal dialysis can only be provided for long and often enough if it is provided during sleep, and thus ensuring optimal ‘living time’
… But how?
Let us think about ‘time’ and ‘frequency’
The Key Question
If better dialysis means increasing time, frequency or, best of all, both … is there a way to do that that is not lifestyle-intrusive?
Time
Daytime dialysis time beyond 4-5 hrs is ‘unacceptably intrusive’ for most patients so … the only viable way to increase dialysis time is to perform dialysis during body ‘down-time’ … i.e. during sleep
Haemodialysis while asleep has long been ‘off-limits’, but … improvements in technology with more creative thinking and solutions to the instability of blood pressure … have made night-time dialysis safe
... see SAFETY ON NHHD and DIALYSIS ISSUES
Frequency
Daytime dialysis frequency beyond 3-4 treatments/wk is also ‘unacceptably intrusive’ for many patients so, the best way to increase frequency is to dialyse more often.
This can be done either …
by shortening the duration of each dialysis … i.e. short (2hr), daily (6days/wk) dialysis (6x2 HD)
by doing dialysis at night, while asleep, so that the higher frequency of dialysis sessions is masked by being done during sleep
With short, daily dialysis, dialysis exposure/wk is the same as for conventional 3x4 HD - it just turns the 4x3 = 12 hrs into 6x2 = 12 hrs
Short, daily HD (6x2) has both advantages and disadvantages
As dialysis efficiency is maximal at the start of dialysis, 6x2 HD is more efficient than 4x3
But ..
Greater travel time to and from the dialysis centre limits the appeal of short, daily HD unless it, too, is done at home
Time and Frequency
Increasing daytime frequency and time makes during-the-day dialysis totally impractical but … using the night and dialysing while asleep is the clear and only practical way to increase both time and frequency
AND
This use of ‘nocturnal’ or ‘overnight’ time
is now possible and safe
due to better equipment and safety options
see SAFETY ON NHHD
Nocturnal haemodialysis (NHHD) is both safe and practical yet leaves the waking hours undisturbed
Increasing time and frequency raises dialysis efficiency. Doubling both the number of treatments/wk from 3 to 6 and the duration of each treatment/wk from 4 to 8 increases the efficiency of waste/fluid removal 4 fold
This 4 fold increase in efficiency allows:
The blood flow rate (pump speed) to be reduced
The dialysis fluid flow rate to be slowed right down
Dialysis becomes almost ‘subliminal’
And … the circulation sighs a heart-felt ‘thank you’
The following graphs show the effect that increasing the duration and/or frequency of dialysis has on the build-up and removal of fluid and wastes.
I have used S.Creatinine measured in mmol/l (SI units) as the ‘y’ (or vertical) axis … but it could represent any waste (or fluid volume) which accumulates and then requires removal during dialysis
Schematic diagram (4hrs x 3/wk) = Conventional (4x3) Haemodialysis
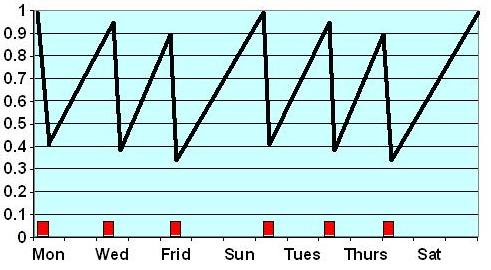
Waste levels and blood volume fall rapidly over each 4 hr HD (represented by the red bars) then rise again over 44 hrs (midweek) or over 68 hrs (weekend) … the cycle recurring the next week
Schematic diagram (2hrs x 6/wk) = Daily (short hour) Haemodialysis
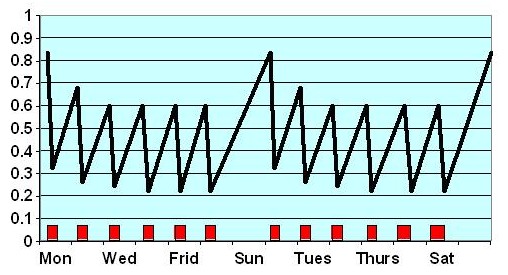
Waste levels and blood volume fall rapidly over each 2 hr HD (represented by the red bars) then rise again over 22 hrs (midweek) or over 46 hrs (weekend) … the cycle recurring the next week
(continued in the next ‘Part’)
Authored by Prof
John Agar. Copyright © 2012
Nocturnal Haemodialysis Program, Barwon Health.
All rights reserved. Revised: July 1st 2012