Dialysis Issues
Blood Pressure
and
Ultrafiltration in Dialysis
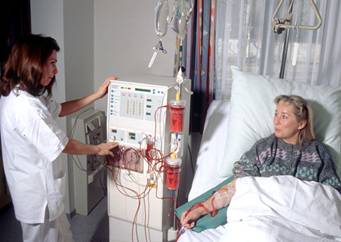
(Click here to view the large text version of this page.)
When thinking about fluid in a dialysis patient, several principles apply …
Fluid taken in, stays in
For most haemodialysis (HD) patients…
fluid into the mouth means fluid in the body
… with no way of it getting out again … except by dialysis.
You see…
Most HD patients pass insufficient urine to keep up with a comfortable fluid
intake
Some are lucky and still make a reasonable volume … but this is the minority of
patients.
Fluid restriction is the worst restriction most HD patients must face
Fluid restriction can be even more difficult for diabetic patients where
high blood sugars aggravate an already raging thirst
Drink too much fluid and risk ‘drowning’ in excess body fluid
As any fluid ‘taken in’ by drinking will stay ‘in’ until removed by the next HD,
the ‘weight gain’ that occurs between HD treatments is not true body
weight gain but, rather, reflects the amount of fluid gained in excess of
any fluid lost since the last dialysis.
This fluid gain:
Swells the blood volume
Distends the blood vessels
Raises the blood pressure
Wets the lungs (sometimes to the point of near-drowning)
Strains the heart and makes it weaker, like a repeatedly over-stretched rubber
band
The sad facts of a typical dialysis day (for most) …
The patient struggles in for HD on a Monday morning after a ‘long break’, that
weekend off for dialysis staff that forces a 68 hour break for without dialysis
on each and every facility-based dialysis patient
…
The arrival scenario
…?
The patient is short of breath with a ‘thumping’ heart and a 4 kg weight gain in
excess of the weight recorded at the end of the previous Friday’s dialysis … and
remember: a 4 kg weight gain equates to a 4 litre retention of ingested fluid
The dialysis plan …?
Remove 4 litres over 4 hours HD … or about 1 litre/hour for every hour of
dialysis
The dialysis result …?
Cramp, nausea and a horrible ‘flat’ - that awful moment when the blood pressure
drops and the eyes roll back in a dead faint
The treatment response …?
A frantic ‘revival’ effort with intravenous (IV)
fluid – when the whole object of the
session has been to remove 4 litres of fluid
The treatment outcome …?
The patient goes home, washed out, exhausted and thirsty-as-hell.
The rest of the day is ‘written off’ to allow recovery
Meanwhile …
The patient immediately starts to drink fluid (when knowing its wrong) to slake
a raging thirst.
Why …?
Because a rapid reduction of blood volume stimulates

And …
Thirst is a powerful, primitive, primal survival
mechanism
Thirst simply cannot be resisted – no matter how much the patient tries.
The inevitable result …?
Another 4 kg (4 litres) is gained and … it all starts over again
With 6 night/week NHHD, it isn’t like that at all …
1. Imagine dialyzing (but while you sleep) … for 8-9 hrs out of every 24 hrs
As NHHD is for 8-9 hours and not just 4, there more than twice as long to remove any
excess fluid
2. Imagine dialyzing every 24 hrs, not just every 48-72 hrs
As NHHD is pretty much every night (6 times/week and not 3 times/week), fluid is also
being removed twice as often
Do your mathematics ... it’s quite simple really …
Twice as long + twice as often = a 4 times slower rate of fluid removal
This means dialysis which is four times as gentle
Ultrafiltration, what is it?
Ultrafiltration is the process by which the artificial kidney (the dialyser)
removes fluid
The rate at which fluid is removed is called the ultrafiltration rate
(UFR)
The more fluid (weight) gained from one dialysis to the next – the higher the
UFR during the next dialysis that is needed to remove that fluid.
The higher the UFR, the greater the risk of symptoms during or after dialysis …
cramps, nausea, vomiting, dizziness, thirst and ‘going flat’
The three fluid ‘compartments’ of the body
What follows now is quite complex … so, take this bit slowly. Even re-read it a
few times … but it IS important you try to understand this bit …
Ok … here we go …
The fluid contained in the body is divided into 3 main ‘compartments’
1. There is the fluid contained within the body’s cells – this is called
intracellular fluid
2. There is the fluid contained in the tissues and spaces that surround the
cells – this is called the extracellular fluid
3. There is the fluid contained within the blood vessels (arteries, capillaries
and veins) – this is called the blood plasma
The fluid (or body water) contained in these three compartments can move from
one to the other – especially if one compartment suddenly loses some of its
fluid volume – and is shown in the next diagram …
Cells
Interstitial
space
Blood vessel and plasma


![]()

|
|

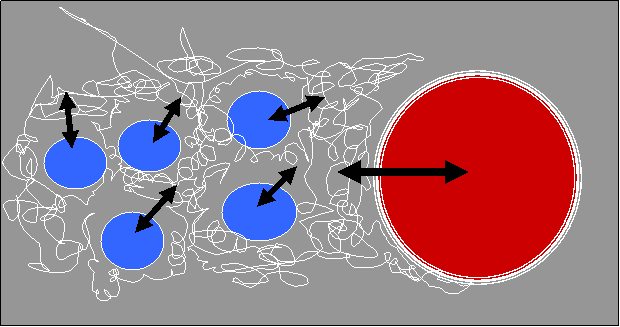
Movement from
compartment to compartment
Although fluid normally moves and balances between each of these three
compartments, the rate at which it
moves is ‘speed limited’.
If fluid is removed from any one of the three compartments (the cells, the
extracellular space or the blood), fluid will ‘seep’ from the other two
compartments to the depleted one to replenish it and to restore the balance
across all three.
If fluid is removed from the blood compartment, fluid will then slowly seep into
the blood from the extracellular space to replenish it.
In turn,
cellular fluid will then replenish the extracellular fluid – re-creating a
balance across all three compartments but with an overall reduction in total
body fluid by the amount first removed from the blood.
But … the rate at which these ‘fluid shifts’ can occur has a ‘speed limit’.
This speed limit is about 0.4 litres/hr … give or take a little.
Exceed the speed limit … and pay the price!
If fluid is removed from the blood stream by ultrafiltration on dialysis at a
rate greater than 0.4 litres/hr, the extracellular fluid will not
be able to replace it fast enough to maintain a balance
Furthermore, the cellular fluid will also fall behind in replenishing the
extracellular fluid
The balance will be upset and the blood volume will begin to fall
The more the UFR exceeds 0.4 litres/hr, the faster the blood volume must fall
Ultimately, the blood pressure will begin to destabilize and will fall or
‘crash’ … and this will create a ‘flat’ on dialysis
Now … back to our fluid-soaked patient
Remember our typical HD patient? … 4 kg (litres) overloaded with fluid and with
only 4 hrs (or less) in which to remove it
Mathematics calculates a UFR of 1 litre/hr from the blood compartment
This UFR exceeds the capacity of the extracellular fluid to replace it by ~0.6
litres/hr
The blood volume will thus drop by ~0.6 litres/hr, every hour of dialysis
Over 4 continuous hours, the blood volume will thus fall by ~2.4 litres
This is like sustaining a massive ‘bleed-out’ every 2nd day
… now you can understand why conventional, infrequent (3 x week), fast (4hrs or
less) haemodialysis ‘knocks people
around’ as much as it does!
The incredible gentleness of NHHD
NHHD is dialysis for twice as long and twice as often.
There is ½ the time to drink in between dialysis sessions … so the fluid gain is
½ as much
The dialysis session runs twice as long … so there is twice the time to remove ½
the amount of fluid
UFR on NHHD is therefore ¼ as severe … dialysis for twice as long and twice as
often
Typically, the UFR of NHHD is ~0.2 to 0.25 litres/hr – and this is well within
the ‘speed limit’ at which the extracellular fluid can replenish the blood
volume
And
so …
the blood volume cannot fall
the blood pressure cannot collapse
the dreaded ‘flats’ of conventional HD cannot occur
Dialysis at night becomes safe because:
The fluid removal rate is slow
The blood volume does not contract
The blood pressure doesn’t fall
‘Flats’ do not happen
Saline ‘revival’ is never required
Thirst is not stimulated
Excess weight gain is thus avoided
Conclusion
…
With NHHD, no-one need be at hand to ‘revive’ you from a ‘flat’, because ‘flats’
and ‘revival’ are no longer issues.
This makes dialysis safe to perform while asleep and makes NHHD safe for single
people at home
This makes NHHD a revolution like no other in dialysis history as long-held
dialysis theory is turned on its head.
Authored by Prof John Agar. Copyright © 2012
Nocturnal Haemodialysis Program, Barwon Health.
All rights reserved. Revised: July 1st 2012